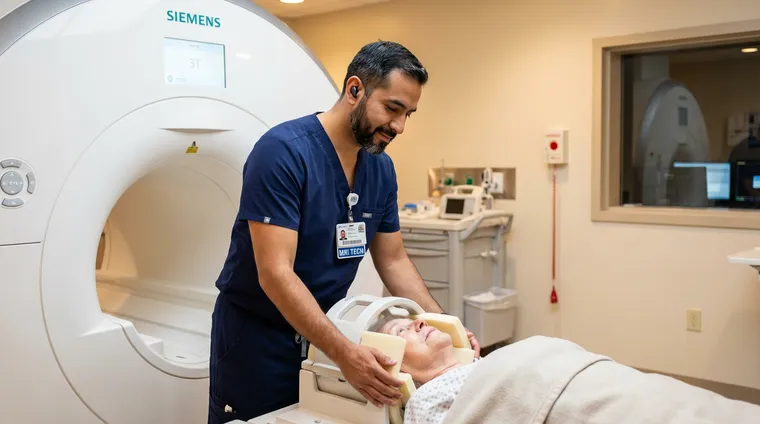
What Being an MRI Technologist Actually Feels Like
An MRI technologist’s typical day involves 8–12 hour shifts scanning 15–25 patients, splitting time between patient preparation (safety screening, positioning, IV placement for contrast studies), scanner operation (selecting protocols, adjusting parameters, monitoring image quality), and communication (explaining procedures to anxious patients, coordinating with radiologists). Here is what the day actually looks like:
- Screening patients for safety (implants, metal, devices)
- Managing patient anxiety during 30–60 minute exams
- Accurately positioning and repositioning bodies for optimal imaging
- Running protocols and adjusting parameters to optimize image quality
- Collaborating with radiologists, nurses, and schedulers
- Managing pace when the schedule stacks up
The job is about 50% patient interaction and 50% technical execution. not sitting in the dark.
A Typical Day: Hour by Hour
Here’s what a day looks like at different settings.
Outpatient Imaging Center: 7am–4pm Shift
| Time | Activity |
|---|---|
| 6:45am | Arrive early, log in, review daily schedule (14 patients today) |
| 7:00am | Patient 1: Brain MRI. Routine screening, smooth scan, 30 minutes. |
| 7:35am | Patient 2: Lumbar spine. Patient anxious about enclosed space, extra communication needed. 40 minutes. |
| 8:20am | Patient 3: Knee MRI. Quick setup, straightforward exam. 25 minutes. |
| 8:50am | Patient 4: Brain with contrast. Patient late by 15 minutes, schedule compressed. |
| 9:30am | Patient 5: Cervical spine. Motion on first attempt, patient educated on stillness requirements, repeated sequences. Running behind. |
| 10:15am | Patient 6: Shoulder. No issues, back on schedule. |
| 10:45am | Break: 15 minutes. Check messages, reset mentally. |
| 11:00am | Patients 7–9: Brain, lumbar, pelvis. Routine morning flow, staying on time. |
| 12:30pm | Lunch: 30 minutes. May need to shorten if schedule slips. |
| 1:00pm | Patient 10: Abdomen with contrast. Longer exam, requires breath-hold instruction. |
| 1:45pm | Patient 11: Hip arthrogram (contrast injected by radiologist, then MRI). More coordination required. |
| 2:30pm | Patients 12–14: MSK exams. Afternoon push to finish on time. |
| 3:45pm | Final documentation, end-of-day cleanup, handoff notes for next shift. |
| 4:00pm | Shift ends. unless there’s an add-on or a re-scan needed. |
Daily patient volume: 12–16 patients typical for outpatient
Hospital MRI: 7am–7pm Shift (12-hour)
| Time | Activity |
|---|---|
| 6:45am | Arrive, review inpatient list, check any overnight urgent orders |
| 7:00am | Inpatient 1: Brain stroke protocol, patient transported from ICU. Collaboration with nurse. |
| 7:45am | Outpatient 2: Routine spine. |
| 8:20am | Emergency add-on: ER sends patient with possible cord compression. Priority case. |
| 9:00am | Inpatient 3: Abdomen, patient sedated. Requires extra monitoring. |
| 10:00am | Back to scheduled patients. Two routine exams. |
| 11:30am | Challenging case: Patient with pacemaker. conditional, requires cardiology clearance. Delays while waiting for approval. |
| 12:30pm | Lunch: Try to eat, but may get pulled for urgent case. |
| 1:00pm | Afternoon scheduled patients. Mix of inpatient and outpatient. |
| 3:30pm | Pediatric MRI: 8-year-old, anxious. Extra time for coaching and breaks. |
| 4:30pm | Continue scheduled patients. |
| 6:00pm | Last scheduled patient. Wrap up documentation. |
| 6:30pm | Check on any add-ons. Evening tech takes over. |
| 7:00pm | Shift ends. or extends if cases are still running. |
Daily patient volume: 8–15 depending on complexity; hospital volume is less predictable
The Workflow Rhythm
MRI work follows a predictable pattern for each patient, but the details vary constantly.
Pre-Scan Phase (10–15 minutes)
- Review order and history: What’s the exam? What’s the clinical question? Any flags?
- Safety screening: Implants, metal, devices, pregnancy, contrast allergies
- Patient education: Explain what will happen, set expectations about noise and duration
- Change and prep: Patient gowns, removes metal, uses restroom
Scan Phase (20–60 minutes depending on exam)
- Position patient: Coil placement, padding, hearing protection, squeeze ball
- Confirm comfort: Patient should be as comfortable as possible. discomfort causes motion
- Run localizer and set up scan: Verify positioning, plan slices
- Execute sequences: Run protocols, monitor image quality as you go
- Communicate as needed: Check in with patient between sequences, manage anxiety
- Contrast (if applicable): Screen again, administer, run post-contrast sequences
Post-Scan Phase (5–10 minutes)
- Verify images: All sequences complete, quality acceptable, coverage adequate
- Release patient: Help them off table, any post-exam instructions
- Document: Complete records, note any relevant observations
- Reset room: Prep for next patient
The Hidden Time
What schedules don’t show:
- Patient transport delays (especially inpatients)
- Cases that run long due to patient factors
- Equipment issues that need troubleshooting
- Add-ons that disrupt the planned flow
- Documentation catch-up between patients
What “Stressful” Actually Means in MRI
MRI stress isn’t about the technology. It’s about the intersection of:
Patient Anxiety × Schedule Pressure
Anxious patients need more time. The schedule doesn’t have more time. You have to manage patient anxiety enough to get diagnostic images without falling so far behind that everyone’s day is wrecked.
This is the core skill that separates okay techs from great ones.
Safety Stakes × Routine Work
Most days are routine. But every screening could surface a safety issue. You can’t treat screening as a checkbox; you have to stay alert for the one patient whose implant history could cause a problem.
The stress isn’t from constant emergencies. it’s from maintaining vigilance through routine work.
Image Quality × Patient Variables
You can do everything right and still get motion artifacts because the patient couldn’t stay still. The question is: was it preventable with better patient communication? Should you repeat? How many repeats are reasonable?
These judgment calls happen constantly.
Hospital vs. Outpatient: The Real Differences
Outpatient MRI Life
Pace: Fast and steady. 12–20 patients/day, throughput-focused.
Predictability: More predictable schedule. Patients are generally scheduled, ambulatory, and cooperative.
Complexity: Lower on average. Common exams: brain, spine, knee, shoulder.
Hours: Often Monday–Friday, 8–10 hour shifts. Less night/weekend work.
Team: Smaller. May be 1–3 techs running the whole operation.
Stress type: Volume pressure. Keeping pace while maintaining quality.
Best for: Techs who like efficiency, routine, and predictable schedules.
Hospital MRI Life
Pace: Variable. Some slow periods, some chaos. 8–15 patients/day with more complexity per case.
Predictability: Less predictable. ER add-ons, inpatient logistics, equipment sharing.
Complexity: Higher on average. More sedated patients, more pathology, more advanced protocols.
Hours: Often includes nights, weekends, on-call coverage. 8 or 12-hour shifts common.
Team: Larger. Part of a bigger radiology department with more resources and coordination.
Stress type: Unpredictability and complexity. Managing difficult cases and constant interruptions.
Best for: Techs who like variety, don’t mind schedule variability, want to see complex cases.
The Physical Reality
MRI is more physical than people expect.
What Your Body Does
- Standing: Most of your shift, you’re on your feet
- Walking: Back and forth between control room and scan room
- Positioning: Physically adjusting patients, often heavier or less mobile ones
- Repetitive motion: Similar movements repeated many times per day
- Confined space: Working in the scan room, which isn’t spacious
Fatigue Factors
- 8–12 hour shifts without sitting much
- Mental fatigue from constant decision-making
- Emotional fatigue from patient interactions
- Noise (MRI is loud; you’re exposed even in the control room)
Self-Care Reality
Smart techs:
- Wear good shoes (seriously. this matters)
- Take breaks when available
- Stay hydrated
- Develop efficient body mechanics for positioning
- Build mental boundaries between work and home
What a “Good Day” Feels Like
A good day in MRI usually means:
- Patients are cooperative and complete their scans
- You’re not fighting motion on every exam
- The schedule runs reasonably close to plan
- No major safety concerns or equipment issues
- You leave on time feeling competent
The best feeling: When an anxious patient tells you “that wasn’t as bad as I expected” because your patient communication worked. Or when the radiologist comments that your image quality is excellent.
What a “Hard Day” Feels Like
A hard day usually involves some combination of:
- Multiple claustrophobic or uncooperative patients
- Motion artifacts requiring repeat sequences
- Schedule stacking up with no recovery time
- Equipment issues or unexpected downtime
- Stressful safety screening situations
- Running late with no break
- Difficult team dynamics or communication issues
The hard truth: These days happen. They’re not every day, but they’re not rare either. Building resilience and good workflow habits helps you handle them.
Why People Love MRI Work
Despite the challenges, many techs find MRI deeply satisfying:
Technical engagement: It’s intellectually interesting. You’re problem-solving with image quality, adapting to patient needs, learning constantly.
Patient impact: You directly help people get diagnoses. Patients thank you for helping them through something scary.
Variety within structure: Each patient is different, but there’s a predictable workflow that creates competence over time.
Job stability: The field is in demand. Skilled MRI techs have options.
Team camaraderie: Good MRI teams support each other through hard days.
Is MRI Tech Work Right for You?
Based on what the day actually involves, MRI fits well if you:
✅ Like patient interaction but don’t want nursing-level medical responsibility ✅ Enjoy technical problem-solving with real-world application ✅ Can stay calm under schedule pressure ✅ Don’t mind physical work (standing, positioning) ✅ Value job stability in healthcare
MRI might not fit if you:
❌ Dislike patient-facing work or coaching anxious people ❌ Want a desk job or minimal physical activity ❌ Get stressed by schedule pressure and unpredictability ❌ Are uncomfortable with high-stakes safety judgment ❌ Need maximum schedule flexibility
Related Reading
Frequently Asked Questions
It can be. Stress comes from schedule pressure, anxious patients, and the responsibility of MRI safety. not from the technology itself. Good patient communication skills and efficient workflow reduce stress significantly. Most techs find it manageable once they build competence.
Outpatient centers typically schedule 12–20 patients per tech per day. Hospital MRI varies more. could be 8–15 depending on case complexity. High-volume sites push higher; specialized sites may be lower but more intensive per patient.
Depends on setting. Hospital MRI often requires nights, weekends, and on-call coverage. Outpatient imaging centers typically run Monday–Friday with more predictable hours. Shift availability varies by market and employer.
Keeping patients still while staying on schedule. Patient movement during scans requires educating patients on what to expect during their exam, but rushing patients increases anxiety. Balancing quality, patient experience, and pace is the core daily challenge.
Neither is objectively better. they're different. Outpatient: faster pace, more predictable hours, routine exams. Hospital: more complex cases, more coordination, more schedule variability. Your preference depends on what type of work energizes you.